What is the Role of Opioids in Cataract Surgery
Opioid-naive cataract surgery patients who receive an opioid prescription within 7 days of surgery are 1.6 times more likely to be using opioids long-term than those who are not prescribed an opioid following cataract surgery.
The majority of cataract surgery patients are considered at greater risk of opioid dependency as age greater than 50 years is a risk factor for post-surgical chronic opioid use following surgery among patients.
Phenylephrine and ketorolac intraocular solution 1%/0.3% (P/K; Omidriai) is used during cataract surgery and intraocular lens replacement and is approved by the FDA for maintaining pupil size by preventing intraoperative miosis and for reducing postoperative ocular pain.
In clinical trials, use of P/K was associated with a 50% reduction in moderate-to-severe pain and a nearly 80% reduction in the need for intraoperative fentanyl; however, there are no existing publications examining whether the use of P/K is associated with a reduction in post-surgical prescribing of opioids.
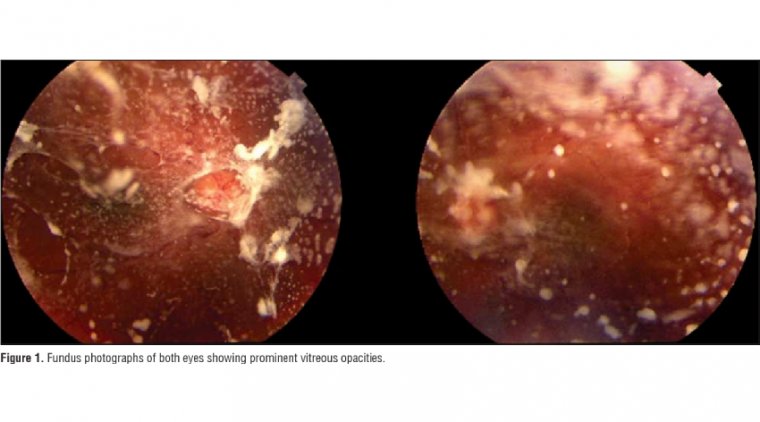
Cataracts are a leading cause of preventable blindness globally. Although care varies between developing and industrialized countries, surgery is the single effective approach to treating cataracts.
From the earliest documented primitive cataract removals to today’s advanced techniques, cataract surgery has evolved dramatically. As surgical techniques have developed, so have approaches to surgical pain management.
With current cataract surgical procedures and advanced technology, anesthesia and intraoperative pain management have shifted to topical/intracameral anesthetics, with or without low-dose systemic analgesia and anxiolysis.
Despite this, pain and discomfort persist in some patients and are underappreciated in modern cataract surgery. Although pain management has progressed, opioids remain a mainstay intraoperatively and, to a lesser extent, postoperatively.
The opioid crisis may have taken a back seat to the COVID-19 pandemic in terms of headlines, but it certainly has not faded. If anything, it has worsened.
Nearly 50,000 people in the United States died from opioid-involved overdoses in 2019, according to the National Institute on Drug Abuse.
Around 21% to 29% of patients who are prescribed opioids for chronic pain misuse them, between 8% and 12% of people using an opioid for chronic pain develop an opioid use disorder, and an estimated 4% to 6% who misuse prescription opioids transition to heroin.
The chances of developing an opioid use disorder depends on factors, such as length of time one is prescribed opioids for acute pain and length of time that people continue taking the drug.
In the United States, the total economic burden of prescription opioid misuse is estimated to be $78.5 billion a year, according to the Centres for Disease Control and Prevention.
It has been reported that opioid-naïve cataract surgery patients who receive an opioid prescription within 7 days of surgery are 1.6 times more likely to be using opioids long-term than those who are not prescribed an opioid following cataract surgery.
Being older than 50 is a risk factor for chronic opioid use following surgery, therefore most cataract surgery patients are considered at greater risk of opioid dependency. It is clear that ophthalmologists, like other physicians, should seek to avoid prescribing opioids whenever possible.
Overcoming adherence challenges
Our cataract patients frequently struggle to adhere to complex postoperative drop regimens. We commonly prescribe 3 different agents—a nonsteroidal anti-inflammatory drug (nSAID), a steroid, and an antibiotic—and expect them to instil these drops as directed.
This is a problem, as we know patients do not use their medications properly, with adherence being a major obstacle.
In fact, 1 study showed that as many as 92% of patients do not correctly instil drops, being hindered by manual dexterity problems and other physical limitations.
We surgeons seek to not only control pain and inflammation but also prevent it to ensure the best patient experience and optimal visual outcomes, particularly in the setting of premium IOLs.
Today we have the option of adopting delivery platforms that require no effort on the part of patients—this is a sea change in our strategies. One such option is preservative-free Dextenza, a dexamethasone 0.4-mg intracanalicular insert made of a resorbable polyethylene glycol–based hydrogel.
The insert is placed within the canaliculus to provide a hands-free and tapered delivery of drug to the ocular surface. It can be inserted preoperatively or intraoperatively, and it takes just 1 minute to do.
The highest concentration of dexamethasone is released during the first 2 weeks, and it slowly tapers over a period of about 1 month. The insert demonstrated a retention rate of 99% in the punctum at day 14 in the studies.
Phase 3 studies showed there were no significant IOP spikes with the dexamethasone 0.4-mg intracanalicular insert compared with placebo.
Certainly, if there was a concern, the insert can be easily explanted. Regarding pain and inflammation in the phase 3 studies, a significantly greater proportion of eyes in the dexamethasone 0.4-mg intracanalicular insert group had an absence of ocular pain and an absence of anterior chamber cells, compared with the placebo group.
Nearing dropless surgery
Many surgeons have found they can go completely dropless by combining Dextenza with intracameral moxifloxacin—particularly if they also use intraoperative ketorolac and phenylephrine (Omidria; Omeros).
The nSAID lasts for 2 to 3 days, which is adequate for a significant number of patients. In my practice, I have moved to using just 1 postoperative drop for 3 to 4 weeks: once-daily bromfenac (Prolensa; Bausch + Lomb).
Dr Eric Donnenfeld and we conducted a study comparing the 3-drop regimen with a dropless or near dropless strategy in 56 patients and found that patients overwhelmingly favoured the latter regimen (96%).
There was no significant difference in patient-reported pain or inflammation as seen on optical coherence tomography, no IOP concerns, and it was less expensive. In other words, the dropless or near dropless approach checked every box.
Although the benefits of sustained-release dexamethasone go well beyond their eliminating need for opioid medications after cataract surgery, avoiding opioids is still a strong and important reason surgeons should consider embracing use of the insert.
As a specialty, we need to remain sensitive to the use of narcotics as well as opportunities we have to proactively reduce pain. The amount of effort it takes to incorporate dropless or near dropless cataract surgery into surgeons’ practice is well worth the numerous benefits they and their patients will reap.