The Surgical Management of Vitreous Opacities
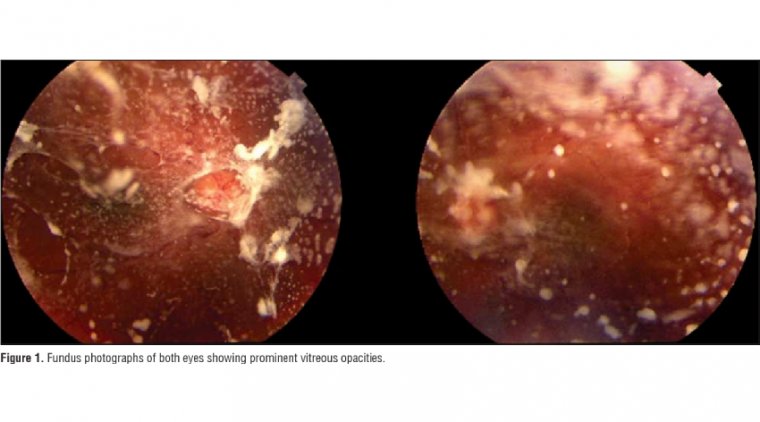
Symptomatic vitreous opacities are increasingly recognized as a significant burden to patient well-being. There is growing interest in the use of vitrectomy or laser treatment to address these problems.
Vitrectomy for the management of severe vitreous opacities is increasingly accepted because of the tremendous relief of symptoms reported by patients. The risks of retinal tear and detachment remain a concern, particularly in patients who have an attached posterior hyaloid.
Yttrium-aluminum-garnet laser treatment of floaters may offer benefit in a subset of patients but appears to be less definitive than vitrectomy, and also may carry significant risk.
The few cells that are normally present in the vitreous gel are located predominantly in the cortex and consist of hyalocytes, astrocytes, and glial cells. Vitreous abnormalities include opacification, liquefaction, and shrinkage.
The term ‘vitreous opacities’ refers to visible structures in the vitreous gel (as opposed to opacities within the vitreous cavity but outside the gel, exemplified by subhyaloid haemorrhage). ‘Vitreous infiltrates’ imply transport of extraneous material through membranes in the retina.
‘Vitreous deposits’ would include such infiltrates as well as substances ‘precipitating’ from within the vitreous itself and becoming visible (eg, synchisis scintillans). ‘Floaters’ usually refer to visual phenomena experienced by the patient.
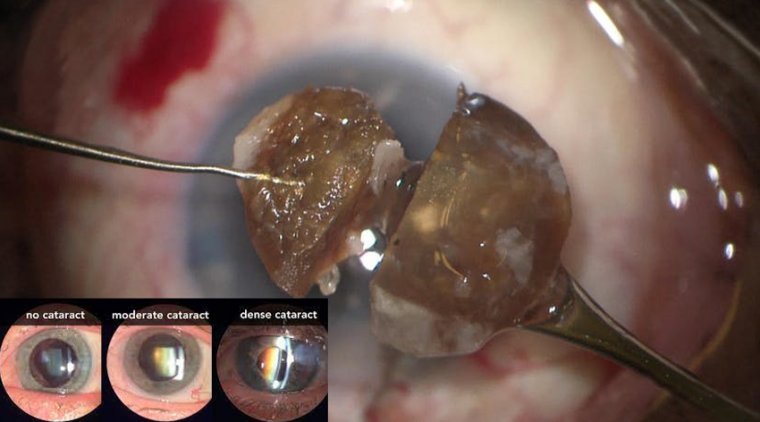
Cataract surgery can be difficult to perform when dense vitreous opacities are present due to the absence of the red reflex.
Even when cataract surgery is combined with vitrectomy, this diffi culty still exists because, in many cases, the view is poor to permit vitrectomy to clear the vitreous opacities before removing the cataract.
Joseph Fong, MD, and Ahmed A. Sallam, MD, PhD, both from the Harvey & Bernice Jones Eye Institute at the University of Arkansas for Medical Sciences in Little Rock, shared their pearls for improving the visualization in these eyes using retroillumination techniques that include a 25-gauge chandelier or a light pipe.
Retroillumination configurations using the chandelier - They described 2 configurations using the 25-gauge chandelier. In the first, the chandelier was directed down toward the vitreous. In the case being demonstrated, the patient had a dense vitreous hemorrhage due to diabetic retinopathy.
Fong recommended that the view often can be improved in this scenario by extinguishing the room and microscope lights and by depending only on the retroillumination provided by the chandelier. In a second case, they demonstrated the view achieved when the chandelier was directed horizontally or toward the lens.
“Directly illuminating the lens from behind provides the surgeon with crisp and detailed visualization of the lens structure and is often very helpful in cases where vitreous hemorrhage is very dense,” Fong said.
Retroillumination using a light pipe In another case of a patient with a dense vitreous hemorrhage from diabetic retinopathy, Fong showed how to maximize use of the light pipe. As in the previous case using the chandelier, maximum visualization was achieved when the lights from the microscope and rooms were turned off.
Fong noted that a light pipe has an advantage compared with a chandelier because an experienced vitreoretinal surgeon has real-time control over the position of the light pipe at all times intraoperatively.
However, the surgeon performs the procedure using 1 hand, which is a major disadvantage when the light pipe is used to provide retroillumination. The surgeon has the option of removing the light pipe to chop the nucleus using both hands.
After the chop procedure is completed, the light pipe can be reinserted to facilitate a better view of the cortex to be removed. “The chandelier and light pipe are both great options to achieve retroillumination and optimal visualization during these challenging cataract surgeries,” Fong said.
“Using the chandelier has an advantage over the light pipe in that the surgeon can use both hands throughout cataract surgery. This frees the surgeon from concerns about the position of the light source and facilitates focus on the details of the challenging surgery.”
Another challenging surgical scenario is in cases of active endophthalmitis. Fong demonstrated insertion of a light pipe into a trocar to retroilluminate the lens during the capsulorhexis.
The light pipe was then inserted through the limbal side port to illuminate the lens during phacoemulsifi cation. “These retroillumination techniques can be used to conquer cataract surgery when many diff erent types of vitreous opacities are present,” Fong concluded.